Uncorking the Truth- How Alcohol Impacts Your Body


In July of 2022 there was an outbreak of the monkeypox virus in the Democratic Republic of Congo which spread to other countries including the United States. Almost a year later, the public health emergency label was lifted as cases declined. In this article we will talk about the history of Mpox, how it spreads, the difference between the two main clades/strains: clade 1 and clade 2, who is at risk, symptoms, and treatment. The sources I used will be linked on the last page.
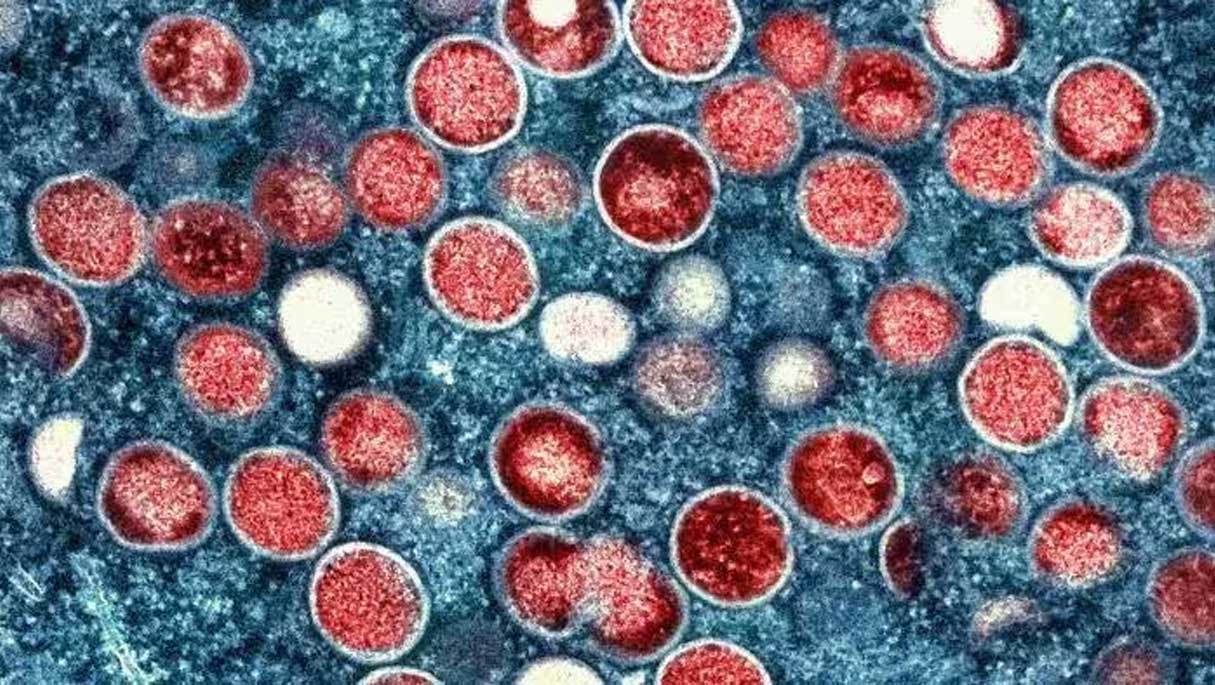 Mpox was first discovered in Copenhagen, Denmark in 1958 when a pox-like disease occurred in monkeys that were kept for research. The first recorded human case of Mpox was in 1970 in what is now the Democratic Republic of Congo. Before 2022, cases of Mpox in other places were rare and usually linked to travel.
Mpox was first discovered in Copenhagen, Denmark in 1958 when a pox-like disease occurred in monkeys that were kept for research. The first recorded human case of Mpox was in 1970 in what is now the Democratic Republic of Congo. Before 2022, cases of Mpox in other places were rare and usually linked to travel.
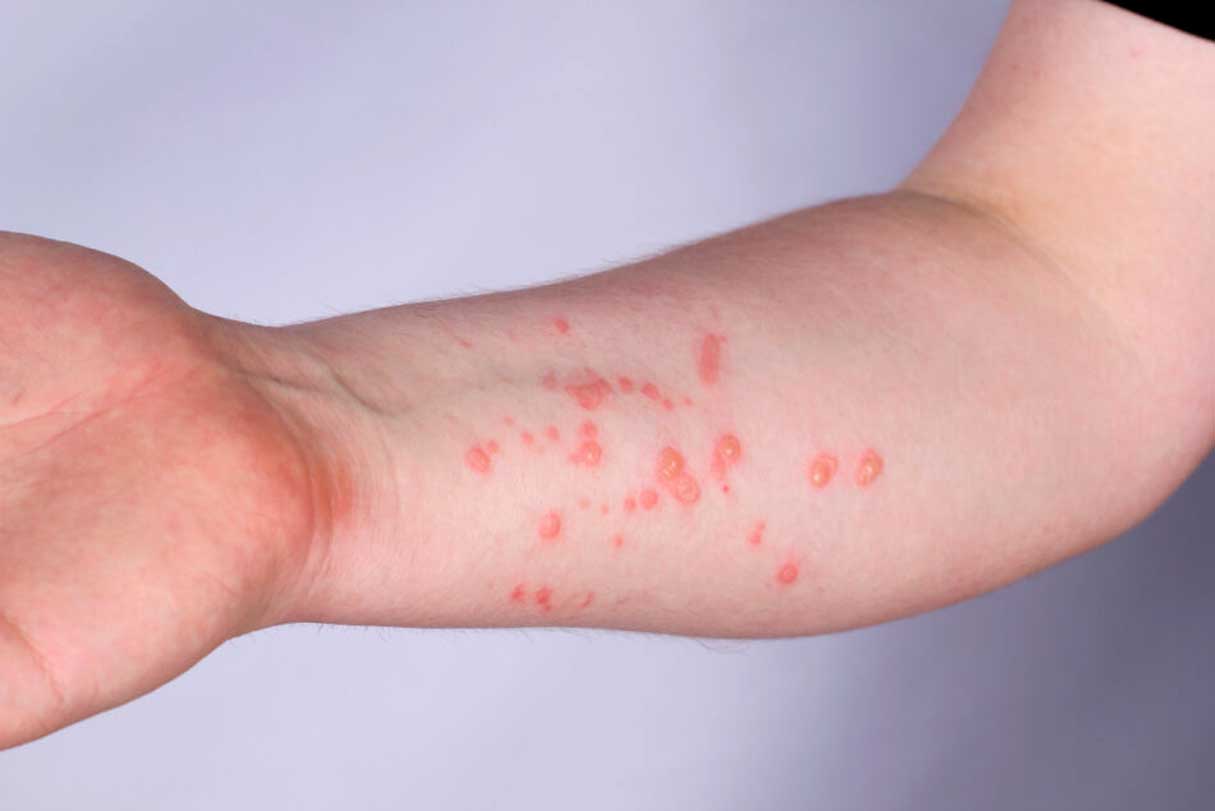
 A person can spread Mpox from the time symptoms start until the rash has fully healed and a new layer of skin has formed. Some people may be able to spread Mpox 1 to 4 days before symptoms. People are considered infectious until all lesions have become crusted, scabs have fallen off, and new skin has formed which can take up to 4 weeks. The virus can also spread during pregnancy to the fetus and during or after birth due to skin-to-skin contact.
A person can spread Mpox from the time symptoms start until the rash has fully healed and a new layer of skin has formed. Some people may be able to spread Mpox 1 to 4 days before symptoms. People are considered infectious until all lesions have become crusted, scabs have fallen off, and new skin has formed which can take up to 4 weeks. The virus can also spread during pregnancy to the fetus and during or after birth due to skin-to-skin contact.
exposure/physical contact with an animal that carries the virus (bites, scratches, or activities like hunting, skinning, trapping or preparing a meal)
Eating contaminated meat
There have been a few reports of Mpox in pet dogs, but these have not been confirmed whether these were true infections or if it was related to surface contamination.
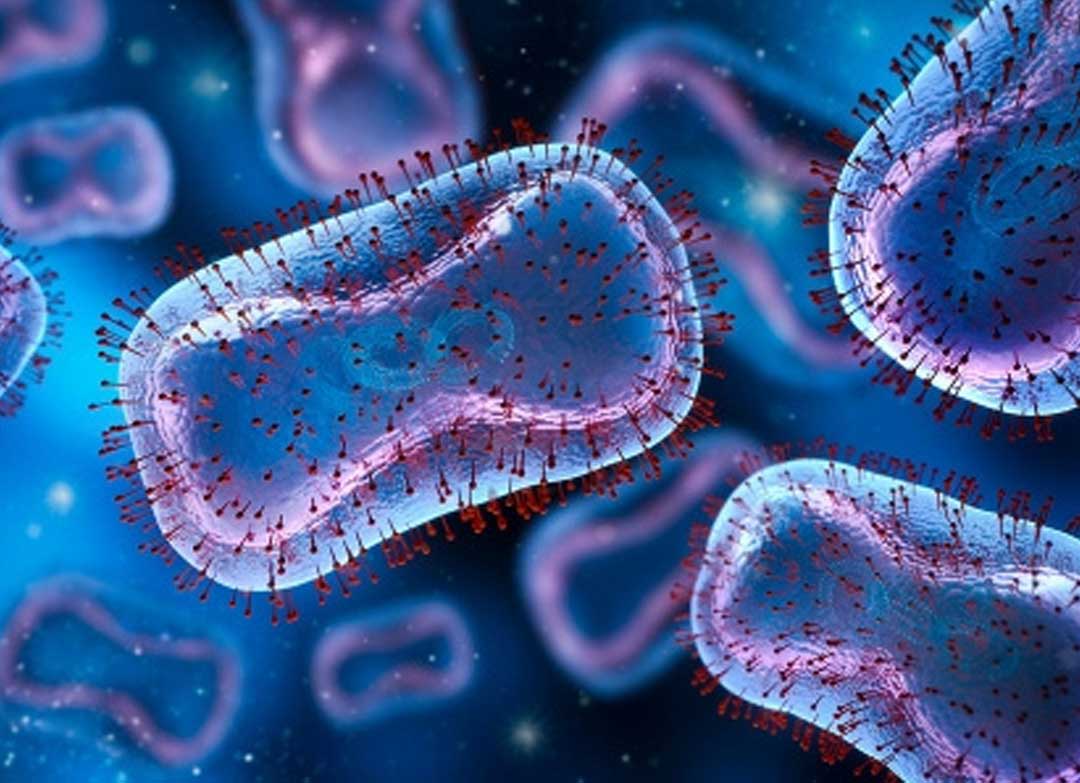 Mpox is a viral illness that is caused by the Monkeypox virus. The Monkeypox virus is part of the same family as smallpox and is also a species of the genus Orthopoxvirus (member of the Poxvirdae family). Mpox is a zoonotic disease which means it can spread between animals and humans. Clade 1 has been historically linked to the Congo Basin while Clade 2 has been linked to West Africa and caused the global outbreak in 2022 and 2023. During the Clade 2 Mpox outbreak that began in 2022, the main transmission route was associated with sexual activity among the LGBTQ+ community. Clade 1 is associated with a mortality of up to 10% and Clade 2 had a mortality rate of less than 1%. Clade 1 causes more severe illness and symptoms than Clade 2. In the Democratic Republic of Congo, over half of reported Clade 1 cases are children. Clade 1 is mostly transmitted through animals who carry the disease, household contacts, close sexual or intimate contact, and contaminated objects. Clade 2; however, is generally not seen in children and is mostly transmitted through same-sex sexual contact.
Mpox is a viral illness that is caused by the Monkeypox virus. The Monkeypox virus is part of the same family as smallpox and is also a species of the genus Orthopoxvirus (member of the Poxvirdae family). Mpox is a zoonotic disease which means it can spread between animals and humans. Clade 1 has been historically linked to the Congo Basin while Clade 2 has been linked to West Africa and caused the global outbreak in 2022 and 2023. During the Clade 2 Mpox outbreak that began in 2022, the main transmission route was associated with sexual activity among the LGBTQ+ community. Clade 1 is associated with a mortality of up to 10% and Clade 2 had a mortality rate of less than 1%. Clade 1 causes more severe illness and symptoms than Clade 2. In the Democratic Republic of Congo, over half of reported Clade 1 cases are children. Clade 1 is mostly transmitted through animals who carry the disease, household contacts, close sexual or intimate contact, and contaminated objects. Clade 2; however, is generally not seen in children and is mostly transmitted through same-sex sexual contact.
It can take several days to a few weeks before you develop symptoms after exposure. Symptoms include:
Rashes can start off as flat, red bumps which will later turn into blisters filled with pus. Not everyone with Mpox develops all symptoms; some may only get a rash with no other symptoms, flu-like symptoms then a rash (some don’t get a rash at all), rashes can be widespread, but some only get a few bumps.
Anyone who comes into physical contact with someone who has symptoms or an infected animal is at risk of getting infected, those who live with infected people have a risk of getting infected, health workers are at risk of exposure. Children often are more likely to have severe symptoms than teens and adults.
The ultimate goal of treating Mpox is to take care of the rash, manage pain, and prevent complications. There are many antiviral medications that have been approved for smallpox that may also help with Mpox. There are also multiple vaccines developed for smallpox that are available globally that could operate for Mpox. Getting vaccinated is recommended for people at high risk of getting Mpox.
Mpox Sources
Some sources may have been used more than once.
One update per week. All the latest news directly in your inbox.